Day 2 :
Keynote Forum
Claudio Blasi
ASLRMB-1D hospital diabetes center, Italy
Keynote: The vagal system as a mediator of the therapeutic effects of bariatric surgery
Time : 10:35-11:10

Biography:
Dr. Claudio Blasi graduated in medicine from Rome “La Sapienza” University at the age of 27 and did a postgraduate specialization in endocrinology at “La Sapienza” School of Medicine. He has been the director of the ASLRMB-1D hospital diabetes center in Rome. He has published more than 30 papers in reputed journals.
Abstract:
Obesity and type 2 diabetes are chronic diseases that respond with difficulty to drug therapies and lifestyle changes. At the origin of this resistance to treatment, an alteration in the functioning of brain sectors in charge of the reward system and of the energy homeostasis, due to a modification of synaptic transmission, has been hypothesized. Overfeeding, presumably beginning as a psychological compulsive search for a rewarding stimulus, turns into food addiction due to the adaptation of synapses in the reward circuit in response to the increased intensity of the inputs (synaptic plasticity). The same would apply to the brain areas responsible for the maintenance of energy homeostasis. The afferent vagal paths transmit to the brain information about ingested food from the digestive tract. Their intermediate station in the brainstem, the vagal nucleus of the solitary tract, has an important role in modulating the metabolic function of the liver and the pancreas. Moreover, they work as a channel for the transmission of information from the periphery to the CNS with regard to both favorable and adverse events. In this way, they influence the synaptic activity of various brain areas through neuroplasticity. The profound anatomical and functional changes in the vagal system caused by bariatric surgery could explain the dramatic improvement in diabetes and the renewed sensitivity to diet by a normalization of synaptic activity. In the future, modulating pharmacologically vagus-vagal synaptic connections or driving brain plasticity via stimulation of the vagus afferents could obtain, “knifelessly”, the same therapeutic effects as surgery.
Keynote Forum
Signe Sørensen Torekov
University of Copenhagen, Denmark
Keynote: Obesity and GLP-1. Obesity pathophysiology and GLP-1 treatment potential
Time : 11:10-11:45

Biography:
Associate Professor Signe Torekov has a strong background in metabolic translational research.
In collaboration with University of California her research has shown that infusion of the natural appetite hormone GLP-1 inhibits appetite and lowers blood glucose (2 first authorships in Diabetes, Obesity and Metabolism (Impact factor (IF) 6.2), 2011 and 2013). During the last three years, her research team has discovered that: 1) obese people have low endogenous GLP-1 response (first author in Diabetes (IF8.4), 2015); 2) weight loss induces a marked increase in GLP-1 response and that this is part of a successful maintenance of weight loss (last author in European Journal of endocrinology (IF4.1), 2016) (major media exposure: front page interview of The Times and live on BBC Today, April 2016 (7 mill listeners), and 3) treatment with GLP-1 analogues facilitate long term weight loss maintenance accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance (Last author in Journal of Clinical Endocrinology and Metabolism (IF6.4) and International Journal of Obesity (IF5.4), 2015). Furthermore, by synergistically integrating metabolic physiology with novel state of the art mass spectrometry based proteomics and metabolomics, in collaboration with Professor Matthias Mann, Max Planck Institute, they have designed a novel experimental approach for clinical translational metabolism in order to identify new health markers in obesity (2. last author in Molecular Systems Biology, (IF 12.3) and last author in Metabolomics (IF3.7), 2016). In addition, Signe Torekov was awarded Major Discovery 2010-2015 for the her first author paper in Diabetes (IF8.4) 2014 where she, together with the research team, showed that Long QT Syndrome patients with mutations in KCNQ1 besides having prolonged cardiac arrhythmia, also have hyperinsulinemic hypoglycemia. More recently, Signe Torekov has shown that Long QT Syndrome patients with loss of function mutations in hERG display exaggerated incretin and endocrine pancreatic function and thus increased risk of symptomatic reactive hypoglycemia. Pharmacological blockade in rats and inhibition of hERG in β and L- cells had similar effects. Hypoglycemia leads to increased propensity for arrhythmias; hypoglycemia may therefore even further increase the risk of malignant arrhythmia in LQTS patients (published in Circulation (IF17) with Dr. Torekov as last and corresponding author).
Abstract:
Obesity impairs almost all aspects of health and is a global challenge to our healthcare system as the prevalence reaches 1 billion humans. Therefore, there is an acute need for better prevention and treatment strategies. Glucagon-like-peptide-1 (GLP-1), secreted from endocrine cells in the intestine upon meal intake, reduces food intake. We have previously shown that: 1) obese people have low endogenous GLP-1 response; 2) weight loss induces a marked increase in GLP-1 response, and 3) treatment with GLP-1 analogues facilitates long term weight loss maintenance (12 kg) accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance. Chronic inflammation is an established part of the pathogenesis of obesity, and activation of macrophages and T cells in the expanded adipose tissue is coupled to the development of a pro-inflammatory state and insulin resistance. Interestingly, emerging evidence identifies GLP-1 as a potentially important immuno-modulator. GLP-1 decreases inflammation-associated gene and protein expression in macrophages and exerts anti-inflammatory actions in adipocytes and endothelial cells as well as potent anti-inflammatory effects in humans.
Keynote Forum
Signe Torekov
Associate Professor
Keynote: Obesity and GLP-1. Obesity pathophysiology and GLP-1 treatment potential
Time : 11:10-11:45

Biography:
Associate Professor Signe Torekov has a strong background in metabolic translational research.
In collaboration with University of California her research has shown that infusion of the natural appetite hormone GLP-1 inhibits appetite and lowers blood glucose (2 first authorships in Diabetes, Obesity and Metabolism (Impact factor (IF) 6.2), 2011 and 2013). During the last three years, her research team has discovered that: 1) obese people have low endogenous GLP-1 response (first author in Diabetes (IF8.4), 2015); 2) weight loss induces a marked increase in GLP-1 response and that this is part of a successful maintenance of weight loss (last author in European Journal of endocrinology (IF4.1), 2016) (major media exposure: front page interview of The Times and live on BBC Today, April 2016 (7 mill listeners), and 3) treatment with GLP-1 analogues facilitate long term weight loss maintenance accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance (Last author in Journal of Clinical Endocrinology and Metabolism (IF6.4) and International Journal of Obesity (IF5.4), 2015). Furthermore, by synergistically integrating metabolic physiology with novel state of the art mass spectrometry based proteomics and metabolomics, in collaboration with Professor Matthias Mann, Max Planck Institute, they have designed a novel experimental approach for clinical translational metabolism in order to identify new health markers in obesity (2. last author in Molecular Systems Biology, (IF 12.3) and last author in Metabolomics (IF3.7), 2016). In addition, Signe Torekov was awarded Major Discovery 2010-2015 for the her first author paper in Diabetes (IF8.4) 2014 where she, together with the research team, showed that Long QT Syndrome patients with mutations in KCNQ1 besides having prolonged cardiac arrhythmia, also have hyperinsulinemic hypoglycemia. More recently, Signe Torekov has shown that Long QT Syndrome patients with loss of function mutations in hERG display exaggerated incretin and endocrine pancreatic function and thus increased risk of symptomatic reactive hypoglycemia. Pharmacological blockade in rats and inhibition of hERG in β and L- cells had similar effects. Hypoglycemia leads to increased propensity for arrhythmias; hypoglycemia may therefore even further increase the risk of malignant arrhythmia in LQTS patients (published in Circulation (IF17) with Dr. Torekov as last and corresponding author).
Abstract:
Obesity impairs almost all aspects of health and is a global challenge to our healthcare system as the prevalence reaches 1 billion humans. Therefore, there is an acute need for better prevention and treatment strategies. Glucagon-like-peptide-1 (GLP-1), secreted from endocrine cells in the intestine upon meal intake, reduces food intake. We have previously shown that: 1) obese people have low endogenous GLP-1 response; 2) weight loss induces a marked increase in GLP-1 response, and 3) treatment with GLP-1 analogues facilitates long term weight loss maintenance (12 kg) accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance. Chronic inflammation is an established part of the pathogenesis of obesity, and activation of macrophages and T cells in the expanded adipose tissue is coupled to the development of a pro-inflammatory state and insulin resistance. Interestingly, emerging evidence identifies GLP-1 as a potentially important immuno-modulator. GLP-1 decreases inflammation-associated gene and protein expression in macrophages and exerts anti-inflammatory actions in adipocytes and endothelial cells as well as potent anti-inflammatory effects in humans.
Keynote Forum
Signe Torekov
Associate Professor
Keynote: Obesity and GLP-1. Obesity pathophysiology and GLP-1 treatment potential
Time : 11:10-11:45

Biography:
Associate Professor Signe Torekov has a strong background in metabolic translational research.
In collaboration with University of California her research has shown that infusion of the natural appetite hormone GLP-1 inhibits appetite and lowers blood glucose (2 first authorships in Diabetes, Obesity and Metabolism (Impact factor (IF) 6.2), 2011 and 2013). During the last three years, her research team has discovered that: 1) obese people have low endogenous GLP-1 response (first author in Diabetes (IF8.4), 2015); 2) weight loss induces a marked increase in GLP-1 response and that this is part of a successful maintenance of weight loss (last author in European Journal of endocrinology (IF4.1), 2016) (major media exposure: front page interview of The Times and live on BBC Today, April 2016 (7 mill listeners), and 3) treatment with GLP-1 analogues facilitate long term weight loss maintenance accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance (Last author in Journal of Clinical Endocrinology and Metabolism (IF6.4) and International Journal of Obesity (IF5.4), 2015). Furthermore, by synergistically integrating metabolic physiology with novel state of the art mass spectrometry based proteomics and metabolomics, in collaboration with Professor Matthias Mann, Max Planck Institute, they have designed a novel experimental approach for clinical translational metabolism in order to identify new health markers in obesity (2. last author in Molecular Systems Biology, (IF 12.3) and last author in Metabolomics (IF3.7), 2016). In addition, Signe Torekov was awarded Major Discovery 2010-2015 for the her first author paper in Diabetes (IF8.4) 2014 where she, together with the research team, showed that Long QT Syndrome patients with mutations in KCNQ1 besides having prolonged cardiac arrhythmia, also have hyperinsulinemic hypoglycemia. More recently, Signe Torekov has shown that Long QT Syndrome patients with loss of function mutations in hERG display exaggerated incretin and endocrine pancreatic function and thus increased risk of symptomatic reactive hypoglycemia. Pharmacological blockade in rats and inhibition of hERG in β and L- cells had similar effects. Hypoglycemia leads to increased propensity for arrhythmias; hypoglycemia may therefore even further increase the risk of malignant arrhythmia in LQTS patients (published in Circulation (IF17) with Dr. Torekov as last and corresponding author).
Abstract:
Obesity impairs almost all aspects of health and is a global challenge to our healthcare system as the prevalence reaches 1 billion humans. Therefore, there is an acute need for better prevention and treatment strategies. Glucagon-like-peptide-1 (GLP-1), secreted from endocrine cells in the intestine upon meal intake, reduces food intake. We have previously shown that: 1) obese people have low endogenous GLP-1 response; 2) weight loss induces a marked increase in GLP-1 response, and 3) treatment with GLP-1 analogues facilitates long term weight loss maintenance (12 kg) accompanied by substantial improvement in metabolic health, compared to diet-induced weight loss maintenance. Chronic inflammation is an established part of the pathogenesis of obesity, and activation of macrophages and T cells in the expanded adipose tissue is coupled to the development of a pro-inflammatory state and insulin resistance. Interestingly, emerging evidence identifies GLP-1 as a potentially important immuno-modulator. GLP-1 decreases inflammation-associated gene and protein expression in macrophages and exerts anti-inflammatory actions in adipocytes and endothelial cells as well as potent anti-inflammatory effects in humans.
Keynote Forum
Lenwood W. Hayman
University of Michigan, USA
Keynote: Keynote: Development and Validation of the Children’s Emotional Eating Scale (ChEES)
Time : 09:05-09:40

Biography:
Lenwood Hayman, Assistant Professor of Public Health at the University of Michigan – Flint, focuses on the psychosocial determinants of eating behaviors in under-privileged communities. Specifically, Lenwood’s research focuses on the assessment of emotional eating (including stressed and bored eating) in preschool-aged children from low-income families. Lenwood has also worked with community-based organizations to demonstrate how increased participation in local food systems correlates with eating a healthier diet. Recently, Lenwood established the Mindful Promotion of Healthy Eating & Learning (Mind-PHEL) research team in which he studies the influence of mindfulness-based activities on healthy eating and positive student learning outcomes. Lenwood is in the process of developing a mindfulness-based intervention to encourage healthy eating behaviors in low-income communities.
Abstract:
Associations between the propensity to eat foods high in sugar and fat in response to negative emotions has been linked to a higher risk of obesity in multiple prior studies in adults. Emotional eating, however, has not been extensively studied in children, particularly among very young children from low-income families. Research suggests that low-income mothers of preschool-aged children believe that children in this age range can eat in response to their emotions, however, they tend to underreport the occurrence of emotional eating for their own children. Such findings could be due, in part, to the fact that the two most commonly-used questionnaires were developed in White, European populations. Due to contradicting evidence regarding the utility of current questionnaires to reliably assess emotional eating in very young children from low-income families in the United States, the focus of the current study was to develop such a scale. Specifically, we used a 2-aim, mixed-methods, cross-sectional design to develop a valid tool for assessing emotional eating at a population level in very young children from low-income families. In our previous work, we qualitatively assessed how mothers from US-based low-income populations conceptualized the construct of emotional-eating in preschool-aged children. We then used that data to develop an inventory of items to capture the salient aspects of emotional eating. These items were assessed by a sample of mothers from the target population for clarity and relatability. Those items demonstrating face- and content-validity, along with the child version of the Dutch Eating Behavior Questionnaire, were then used to collect data from a sample of 200 participants from the target population. Results and conclusions will be discussed in detail during conference session.
- Bariatric surgery for obesity and metabolic disorder | Obesity
Location: 1
Session Introduction
Marek Benes
Institute of Clinical and Experimental Medicine, Czech Republic
Title: Final Results of Multi-Center, Prospective, Controlled Trial of the Duodeno-Jejunal Bypass Liner for the Treatment of Type 2 Diabetes Mellitus in Obese Patients: Efficacy and Factors Predicting a Suboptimal Effect
Time : 15:40-16:05

Biography:
Marek Benes M.D., born 1976 in Prague, where also graduated on 3rd Medical Faculty of Charles University in 2001, in this year started as physician on department of gastroenterology and hepatology in Institute of clinical and experimental medicine in Prague. Main subjects of interest are endoscopy and specially bariatric endoscopy. In present time we have biggest group of patients treated with gastro-jejunal bypass sleeve - Endobarrier in Europe.
Abstract:
Introduction: The global increase in obesity incidence results in an increase of type-2 diabetes mellitus (T2DM). Surgical treatment has proven to be effective; however it carries a high risk of complications. The duodenaljejunal bypass liner (EndoBarrier®, GI Dynamics and EB) is an endoscopic implant that mimics the intestinal bypass portion of the Roux-en-Y gastric bypass. It results in weight loss and improvements in glucose control in obese patients with T2 diabetes mellitus (T2DM).
Aims & Methods: This is a final report of a prospective, controlled, multi-centre study aimed to determine the effectiveness of EB and to identify factors associated with a sub-optimal outcome of EB.
Results: Seventy (70) subjects (45 with an implant, 25 controls) were included in the study. The groups were comparable with respect to age, gender, BMI (mean 41.7 vs. 39.5 kg/m2), T2DM duration (7.8 vs. 8.3 years), HbA1c level (88 vs. 86 mmol/mol) and T2DM treatment. In the EB group, all devices were successfully implanted. Only 6 devices had to be explanted prior to the end of the 10 months study period (bleeding, dislocation and need for ERCP because of choledocholithiasis). The mean procedure time was 17 minutes for an implantation and 16 minutes for an explanation. At 10 months there was significantly greater weight loss and %EWL (19% vs. 7% and 43 vs. 12) and significantly improved long-term compensation of T2DM marker HbA1c (decreased by 25 vs. 10 mmol/mol) in the EB group. T2DM medicinal treatment could be reduced in more device subjects than controls. There was no serious adverse event. Mild abdominal pain and nausea after implantation were experienced by 60% of patients during first 14 days after implantation, 30% of patients during the first month and 10% of patients after one month. Lower initial BMI and lower body height were identified as negative prognostic factors for pain, but positive for efficacy of EB.
Conclusion: The EB is safe when implanted for 10 months and results in significant weight loss and HbA1c reduction. This suggests that this novel device is a candidate for the primary therapy of morbid obesity and T2DM. Lower initial BMI and lower body height could be negative prognostic factor for pain, but positive for efficacy.
Reshma Ramracheya
University of Oxford, UK
Title: Unravelling the role of the gut hormone PYY in diabetes remission and pancreatic islet function following Roux-En-Y gastric bypass
Time : 16:30-16:55

Biography:
Dr. Reshma Ramracheya investigate the regulation and failure of the insulin-secreting beta-cell and glucagon-secreting alpha-cell in normal health and diabetes respectively. As an islet physiologist, She intrigued by how pancreatic islet cells, despite being biochemically similar, are able to respond to nutrients and drugs differently. Type 2 diabetes is a global epidemic with over 300 million sufferers worldwide. It results from a combination of insufficient insulin secretion and over-secretion of glucagon but the role of glucagon as a counter-regulatory hormone in diabetes has been largely overlooked.Her group is investigating the effects of weight-loss surgery and the appetite-regulating hormone peptide tyrosine tyrosine (PYY) on pancreatic islet secretion and in human diabetes. In parallel, they are also studying the mechanism by which the gut hormone glucagon-like peptide 1 (GLP-1) inhibits glucagon secretion in human isolated islets.
Abstract:
Roux-En-Y gastric bypass (RYGB) results in long-lasting remission from type-2 diabetes (T2D) in most cases. Improvements in glucose homeostasis occur within days of surgery, but the mechanisms involved remain unclear. Although pancreatic islets play a fundamental role in glucose homeostasis, the impact of RYGB on islet architecture and secretory properties has not been studied thoroughly. T2D is a bihormonal disease characterised by both insufficient insulin secretion and impairment in glucagon regulation. Whether RYGB can correct both hormonal secretory defects remain unexplored.
Using the Goto-Kakizaki (GK) rat model of T2D, we have explored whether RYGB affects islet structure and glucose-stimulated insulin secretion (GSIS) and glucagon release. RYGB restored ‘distorted’ islets from diabetic rats to spheroidal shape as in healthy animals. Compared to the sham-operated animals, RYGB normalised glucose-dependent glucagon and insulin secretion. Thus, islets from RYGB rats exhibited markedly enhanced insulin secretion at 20mM glucose and complete restoration of glucose-induced suppression of glucagon release.
Culture of isolated islets with serum from RYGB animals resulted in improved insulin and glucagon secretion, in support of a humoral factor which remains conserved in serum. These effects were reversed following immuno-neutralization of the gut hormone peptide tyrosine tyrosine (PYY) but persisted in the presence of a glucagon-like peptide-1 (GLP-1) receptor antagonist. Chronic (60-72h) treatment of islets with synthetic PYY enhanced GSIS in a NPY1-receptor-dependent manner. PYY application also restored GSIS and normalised impaired glucose-induced glucagon release in islets from severely diabetic GK rats and human donors with T2D. These data provide a novel mechanistic insight on the effect of RYGB in diabetes and highlight that the mechanism behind the improvement of islet function is dependent on PYY, and not GLP-1.
These findings imply that a pharmacological agent enhancing PYY release or its action could provide an effective and non-surgical therapy for T2D.
Sukaina Jaffar
Department of Surgery, Nepean Hospital
Title: Multi-dimensional validated reporting of dysphagia post sleeve gastrectomy

Biography:
Abstract:
Background: Few studies have reported the prevalence of dysphagia, as its own clinical entity in the bariatric population; without being examined under the umbrella of gastro-oesophageal reflux disease. This is compounded by studies not outlining methodologies used to assess dysphagia. Moreover, varying follow-up periods and different bariatric procedures have led to conflicting results.
Objectives: To assess the prevalence of dysphagia using a statistically robust patient-reported tool, Dysphagia Handicap Index (DHI) post Laparoscopic Sleeve Gastrectomy (LSG). DHI is a validated tool which additionally measures the handicapping effects of dysphagia on emotional and functional domains of living. Methods: DHI questionnaire was administered to 124 patients who underwent LSG at least 1 year prior. Post-operative weight, change in BMI, percent Total Weight Loss (%TWL) and percent Excess Weight Loss (%EWL) were calculated. Physical, emotional and functional subscales were analyzed separately and altogether. Three additional questions were added to the DHI to delineate oesophageal dysphagia.
Results: Average pre-operative weight and BMI is 123.8 kg and 43 kg/m2, respectively. Median %TWL and %EWL are 32% and 76.2%, respectively. An average reduction in BMI value of 14 kg/m2 was found. 41% of our cohort reported to mild dysphagia and 54% reported moderate to severe dysphagia based on the Modified DHI Score (DHI+Oesophageal Specific Dysphagia Score). No patient required corrective intervention. Patients reporting higher DHI scores were less likely to achieve the median TWL of 35.4 kg (OR 0.40, 95% CI 0.17-0.91). Dysphagia is a common symptom reported in our cohort and was found to have an impact on weight loss outcomes.
Conclusion: Prospective, single-institution analysis using a validated tool reveals post-operative dysphagia to be a common clinical entity in our population with functional and psychological influences.
Biography:
Attila Seyhan was an Assoc. Prof. at the Translational Research Institute for Metabolism and Diabetes, Florida Hospital, an Adjunct Prof. at Sanford-Burnham Prebys Medical Discovery Institute, Orlando, FL and a Research Affiliate with the Department of Chemical Engineering, MIT.
Previously he was in pharmaceutical (Pfizer, Wyeth) and biotech (OpenBiosystems, Dharmacon, Somagenics) in leading positions. He has 16+ years of experience in drug/target/ biomarker discovery and development, preclinical/clinical Translational Research in metabolic diseases/diabetes, cancer, inflammation & immunology, and viral pathogens (HCV, HIV, Semliki forest virus) in leading positions. He has published 35+ scientific articles and book chapters and is an inventor/co-inventor of more than 9 issued US patents and several pending applications. He has successfully authored/co-authored over 14 grant proposals totaling $6.2 million, including a Biodefense grant from the US Department of Defense, NIH and Pharma. He has earned several awards including a doctoral fellowship from NATO, Pfizer Excellence Award for contributions towards Biomarkers of Lupus Disease Study
Abstract:
- Young Researchers Forum
Session Introduction
Maryam Pishsaraeian
Meshkat School, Iran
Title: The evolution of aerobic activity on the level of IgA immunoglobulin in female teenager students
Time : 16:45-17:10

Biography:
M Pishsaraeian has completed her MS degree in Exercise Physiology from University of Mazandaran, Babolsar. Iran. She is a teacher of Sport Science in High School of Tehran city and her field of interest is the evaluation of effects of sport and exercise on psychological and physiological factors.
Abstract:
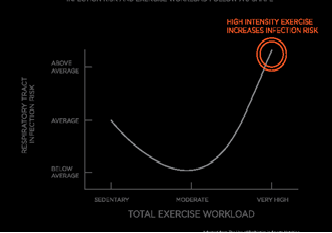
Obesity is a major problem in many societies. One of the proposed solutions for the treatment of obesity is exercise. Exercise has complex effects on immune system. One of most important immunoglobulins in mucus is IgA that protect the body against microorganisms. The aim of this study was to evaluate the effect of aerobic exercise on the levels of IgA and total protein in salivary of female teenager students. 20 female healthy volunteer students (age 12-13) without any infection, using drug, cardiovascular diseases and with healthy diet randomly divided into control (n=10) and aerobic activity (n=10) groups. Before the exercise saliva samples were taken from each student and kept in suitable condition. Aerobic activity group performs the Shuttle Run Test for exercise and control group has no activity. After finishing the exercise the samples were collected and sent to laboratory for analysis. For detection of IgA the ELISA kit essay was used and the Bradford protein essay was used for the detection of total protein. Our results have indicated that in comparison with pre-test and post-test of aerobic activity group, the level of IgA concentration was significantly (P≤0/05) decreased but the total protein was increased (P≤0/05) significantly. There has been no significant change in the level of IgA between two groups. It is recommended that duration, type and intensity of physical activity be considered for prevention of infection.
- Obesity
Session Introduction
Sandra Jumbe
Doctor
Title: Post-surgical cliff after bariatric surgery: accounts of patients and their health care professionals

Biography:
Sandra is a health psychologist with research interests in chronic disease management and smoking cessation. She recently completed her doctorate in health psychology at the University of the West of England in Bristol, UK. She previously worked in the National Health Service (NHS) as a primary care and mental health researcher, an assistant psychologist and in research governance. She has also delivered consultancy work developing tailored stress management interventions within organisations and group settings. Alongside her research work, Sandra also works as a general advisor for the London Research Design Service team based at Queen Mary University, which involves supporting health professionals and research teams within the North East London area to develop their research ideas into full funding applications to the NIHR and other peer reviewed funders
Abstract:
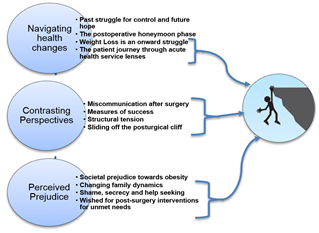
Statement of the problem: The superiority of bariatric surgery for improving medical outcomes in severely obese individuals when compared to other weight loss interventions remains undisputed. However, knowledge about the psychological impact of the procedure on people’s lives is limited. Recent systematic reviews have shown persisting disordered psychosocial wellbeing after surgery when compared to control groups, especially after long-term monitoring, suggesting need for psychological support and longer term postoperative research on psychological outcomes. Research literature infers limited understanding regarding the postoperative lived experience from the patient perspective. This may form a barrier in health professionals’ understanding of this patient group’s postoperative ongoing needs. This study aimed to capture patients and health professionals’ accounts of the postoperative bariatric surgery experience, exploring concordance between the two groups to gauge awareness of patients’ subsequent health needs
- Bariatric surgery for obesity and metabolic disorder
Location: Olimpica 4
Session Introduction
Sukaina Jaffar
Nepean Hospital, Australia
Title: Correlation between Laparoscopic Sleeve Gastrectomy outcomes and Mental Health
Time : 15:50-16:15

Biography:
Abstract:
Sukaina Jaffar
Nepean Hospital, Australia
Title: Correlation between Laparoscopic Sleeve Gastrectomy outcomes and Mental Health

Biography:
Abstract:
- Obesity
Location: Olimpica 4
Session Introduction
Dr. Sandra Jumbe
Queen Mary University of London, UK
Title: Post-surgical cliff after bariatric surgery: accounts of patients and their health care professionals

Biography:
Sandra is a health psychologist with research interests in chronic disease management and smoking cessation. She recently completed her doctorate in health psychology at the University of the West of England in Bristol, UK. She previously worked in the National Health Service (NHS) as a primary care and mental health researcher, an assistant psychologist and in research governance. She has also delivered consultancy work developing tailored stress management interventions within organisations and group settings. Alongside her research work, Sandra also works as a general advisor for the London Research Design Service team based at Queen Mary University, which involves supporting health professionals and research teams within the North East London area to develop their research ideas into full funding applications to the NIHR and other peer reviewed funders
Abstract:
- Types of bariatric surgery
Location: Olimpica 4
Session Introduction
Matteo Catanzano
Department of Surgery, Aberdeen Royal Infirmary, Aberdeen, UK
Title: Stapless laparoscopic sleeve gastrectomy: reasoning and technical insights
Biography:
Dr. Matteo Catanzano has completed his MBChB, at the University of Glasgow, where he started carrying out research, something he has continued now that he is in his second year of foundation training, as a part of the Bariatric Surgery team in the Aberdeen Royal Infirmary.
Abstract:
Introduction: Laparoscopic sleeve gastrectomy (LSG) with staple line reinforcement (SLR) is a popular and safe treatment option for morbid obesity, yet its benefits remain inaccessible to many, especially in developing countries, due to the high cost of the equipment required.
Objective: Devise and describe a modified, stapless laparoscopic sleeve gastrectomy that is as safe as standard LSG with SLR, but costs less.
Methods: Analysis of the influence of technical adaptations on the outcome of LSG was performed in a case–series of 3 patients. The main modification adapted was performing the closure of the stomach stapless. The primary outcome was the occurrence of leak post-op. The secondary outcomes were: operative time, prolonged hospital stay, % excess weight loss at 6 months and 12 months.
Results: Median operative time and hospital stay were 132 min and 2 days. No post-op leaks were recorded. The median excess weight loss at 6 months was 39% and at 1 year 57.7%.
Conclusion: Stapless LSG is an affordable alternative to the standard LSG techniques, both in terms of financial costs and complications rate
- Gastric Bypass Surgery
Location: Olimpica 4
Session Introduction
Mohos Elemer
Veszprem County Hospital, Hungary
Title: Single centre results after 588 laparoscopic Roux –en-Y gastric bypass and 57 laparoscopic gastric sleeve resections performed in Hungary between 2010 and 2017
Biography:
Mohos Elemer is currently working Veszprem County Hospital, Hungary. He published many articles about his field of Bariatric Surgery in different Journals.
Abstract:
Dr. Aly Elbahrawy
Surgeon, McGill University Health Center Montreal General Hospital.
Title: Laparoscopic wedge resection of gastrojejunostomy for weight recidivism after gastric bypass
Biography:
Dr. Ely Elbahrawy is working in Department of Surgery, and Division of General Surgery, Center for Bariatric Surgery, McGill University Health Center Montreal General Hospital, 1650 Cedar Avenue, Canada.
Abstract:
Background & Aim: Weight recidivism after Roux-en-Y gastric bypass (RYGB) is a common problem. Often, this weight loss failure or regain may be due to a wide gastrojejunostomy (GJ). We evaluated the feasibility and safety of a novel approach of laparoscopic wedge resection of gastrojejunostomy (LWGJ) for a wide stoma after RYGB associated with weight recidivism.
Methods: This is a single-center retrospective study of a prospectively-collected database. We analyzed outcomes of patients with weight recidivism after RYGB and a documented wide GJ (>2 cm) on imaging, who underwent LWGJ between 11/2013-05/2016.
Results: Nine patients underwent LWGJ for dilated stomas. All patients were female with a mean±SD age of 53±7 years. Mean interval between RYGB and LWGJ was 9±3 years. All cases were performed laparoscopically with no conversions. Mean operative time and hospital stay were 86±9 minutes and 1.2±0.4 days, respectively. The median (IQR) follow-up time was 14 (12-18) months. During follow-up, there were no deaths, postoperative complications or unplanned readmissions or reoperations. The mean and median (IQR) BMI before RYGB and LWGJ were 55.4±8.1 kg/m2 and 56.1 (47.9-61.7) and 43.4±8.6 kg/m2 and 42.1 (38.3-47.1), respectively. One year after LWGJ, mean and median (IQR) BMI significantly decreased to 34.9±7.3 kg/m2 and 33.3 (31.7-35.0) corresponding to a mean %EWL of 64.6±19.9 (P<0.05).
Conclusion: LWGJ is safe and can lead to further weight loss in patients experiencing weight recidivism after RYGB with a wide GJ (>2 cm). Long-term follow-up is needed to determine the efficacy and durability of LWGJ and compare its outcomes with other endoscopic/surgical approaches for weight recidivism after RYGB with a documented wide GJ.
